Health insurers submit rate filings annually to state regulators detailing expectations and rate changes for Affordable Care Act (ACA)-regulated health plans for the coming year. A relatively small share of the population is enrolled in these plans (compared to the number in employer plans), but these filings are generally more detailed and publicly available. These filings provide insight into what factors insurers expect will drive health costs for the coming year.
For 2024, across 320 insurers participating in the 50 states and DC, this analysis shows a median proposed premium increase of 6%. Based on a more detailed analysis of publicly available documents from 58 insurers, growth in health care prices stood out as a key factor driving costs in 2024. In addition to inflation, insurers also mention changes in pandemic-related costs and the unwinding of Medicaid continuous coverage, though the latter are having a small, if any, effect on premiums.
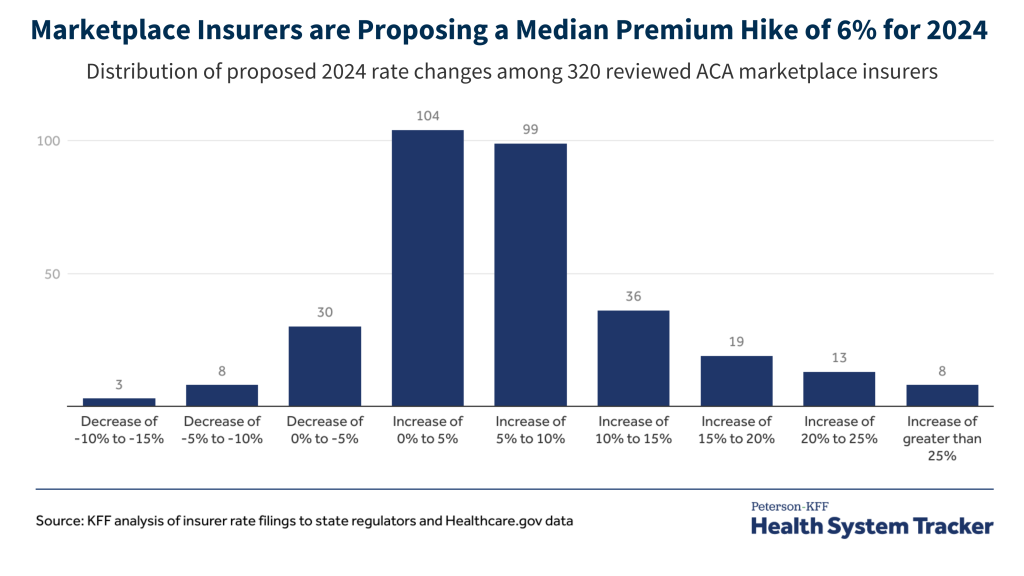
Among 320 ACA Marketplace participating insurers nationally, premium changes range from a drop of –15% to an increase of 100%, but most proposed premium changes for 2024 fall between about 2% and 10% (the 25th and 75th percentile, respectively). Of the 320 filings, 41 insurers proposed decreasing premiums. On the other end of the spectrum, 76 insurers requested premium increases greater than 10%. These filings are preliminary and may change during the rate review process. 2024 rates will be finalized in late summer. A table in the appendix shows proposed premium increases by state and insurer.
The rate increase for an insurer is a weighted average across all of its products within a state (i.e., bronze, silver, gold and platinum plans). These weighted average premium changes will differ from the percent change in the benchmark silver plan, which is the basis for federal subsidies. Most enrollees in this market receive a subsidy and are not expected to face these premium increases. However, premium increases could result in higher federal spending on subsidies.
What’s driving 2024 premium changes?
The chart above shows premium changes for 320 insurers across all 50 states and DC. For the subsequent sections, this analysis focuses on a subset of these rate filings (58 insurers across 11 states and DC) in more detail to understand the factors driving premium changes in 2024. These insurers and states were selected because they have earlier and more transparent (less redacted) public reporting of proposed rate justifications. For context, though, the 58 insurers reviewed in this section have somewhat higher proposed rate increases, with a median of 9%.
Inflation
As is the case in most years, medical trend – which includes growth in prices paid by insurers for medical services and medications, as well as growth in the utilization of health care – is a key driver of premium growth in 2024. Many insurers expect utilization to grow relative to 2022, but price growth is generally playing a larger role in medical trend than utilization is.
Of the insurer rate filings reviewed in detail, and when an annualized trend was publicly available, the median medical trend was 8%, with most reporting trend in the 7-9% range.
“The primary driver of the premium increase is the increases in the cost of healthcare. The increases are associated with increases in the “unit” cost of services primarily from hospitals, physicians, and pharmaceutical companies, coupled with increases in the consumption of services, or “utilization”, by members.” – Anthem Health Plans, Kentucky
While health sector prices typically outpace price growth in the rest of the economy, the last two years have been an exception. Recent medical price growth has been similar to past years, while growth in prices in the rest of the economy has grown at a faster than usual pace. As contracts between insurers and providers are typically negotiated for a year or more, medical inflation often lags that in the rest of the economy.
Looking ahead to 2024, many insurers are expecting broader economic inflation to flow through to the health system and put upward pressure on premiums.
“Significant inflation in the cost of goods and services in all sectors of the economy has had a profound impact on the cost of medical services, and BCBSRI expects to see substantial increases in provider unit costs for 2024.” – Blue Cross Blue Shield of Rhode Island
“We expect unit cost trends to be higher in 2023 and 2024 due to inflation, supply shortages and labor shortages. Inpatient hospital cost per day trends will be increasing as hospitals seek to recover from 2022 financial losses.” – Kaiser Foundation Health Plan of Washington
“Health insurance premiums must correspond with the cost of our members’ medical care, which continues to rise at an unparalleled rate year after year and is projected to increase significantly in 2024. Rising medical costs are the primary driver of our proposed individual rates and increase requested premiums by 19.1%.” – Highmark, New York
In addition to driving up prices paid by insurers to providers, inflation is also putting upward pressure on insurers’ administrative costs, such as their own staffing costs.
“Blue Cross VT is increasing base administrative costs (see section 3.8.7), which has the effect of increasing the premiums by 0.1 percent for individuals and 0.3 percent for small groups. This modest increase reflects current and expected inflationary levels.” – Blue Cross Blue Shield of Vermont
COVID-19 and the end of the Public Health Emergency
This year, as they did in prior years, insurers acknowledge there is still uncertainty surrounding the future of the pandemic. With the end of the Public Health Emergency (PHE) this year, plans can now charge cost sharing for COVID-testing, which could have a downward effect on insurer costs and therefore a downward effect on premiums. Conversely, the COVID vaccine will be commercialized, meaning increased cost to insurers on a per-dose basis. The use of COVID-19 related prevention and treatment may diminish, though, if severe cases continue to be less common. On net, most insurers that publicly quantify the effect of the COVID-19 pandemic in their filings expect their pandemic-related costs to decrease in 2024, having a small downward effect on premiums.
“MVP is assuming a 10% reduction in Covid testing costs in the projection period due to a utilization decrease, resulting in the removal of $0.31 PMPM. We expect demand for testing to decrease once cost sharing is reinstituted.” – MVP Health Care, VT
“Costs related to COVID-19 decreased significantly in 2022 compared to 2021, and have reached a relatively consistent month-to-month level since March 2022. We expect 2023 and 2024 COVID related costs will continue at this lower level and possibly trend slightly downward as population immunity continues to grow.” – Molina Healthcare of Washington
The pandemic had a significant downward effect on utilization of health care generally early on, particularly in 2020, but insurers are expecting a continued return to more normal levels going forward.
“While 2022 trends are lower than 2021, we expect utilization trends to moderate and return to pre-COVID-19 levels over 2023 and 2024.” – Kaiser Foundation Health Plan of Washington
Few insurers mention pent up demand for the non-COVID care that was missed in 2020, and most of those that do mention it say the level of use they are expecting in the remainder of 2023 and 2024 is consistent with pre-pandemic trends. Very few insurers expect pent up demand to drive up costs in 2024.
Unwinding of Medicaid continuous enrollment
On April 1, 2023, states started unwinding the Medicaid continuous enrollment provision, resulting in at least 3.8 million people being disenrolled from Medicaid as of August 1, 2023. As a result, some people who have been disenrolled and deemed no longer eligible for Medicaid may enroll in the ACA marketplaces, where they may be eligible for subsidies.
About half of the insurer rate filings reviewed do not mention Medicaid disenrollments in their 2024 premium filings. Those that mention the unwinding of Medicaid continuous coverage often say the impact on costs is difficult to predict, so they are not adjusting premiums. Several insurers say there will be an increase in their ACA enrollment, but no effect on market morbidity (i.e., the average health of enrollees), meaning no net impact on premiums.
“Our assumption is that the new members formerly in Medicaid will select a Blue Cross VT plan comparable to the current market share, about 60 percent, resulting in the Blue Cross VT individual market growing by 1,609 members and the Blue Cross VT small group market growing by 1,711 members. We further project that the new Medicaid members will have the same risk score relationship between the carriers as the existing market; therefore, the risk score impact is 1.000 for both carriers.” – Blue Cross Blue Shield of Vermont
A relatively small number of insurers expect the Medicaid unwinding to lead to a sicker group of people signing up for ACA plans, which would then have an upward effect on premiums.
“Medicaid redetermination and an otherwise shrinking market would lead to an increase in market average morbidity as relatively sicker members will enter and healthier members will leave the market.” – BridgeSpan Health Company of Oregon
Other Potential Drivers of Costs
Some other factors that insurers mentioned in their 2024 rate filings, though much less commonly than the factors described above include:
Diabetes and Weight Loss Drugs. Diabetic drugs, such as Semaglutide, are increasingly being utilized for weight loss. Given the increasing cost and use of Semaglutide and related drugs, a handful of insurers mention these drugs as having an upward effect on their pharmaceutical spending.
The Inflation Reduction Act (IRA). The IRA extends pandemic-era enhanced subsidies through 2025, bringing down premium costs for most consumers in this market. Few insurers mentioned the impact of the IRA subsidies on premiums as there has been no change in the amount of the subsidy from last year.
Other federal policy changes do not appear to be driving premiums. Among insurer filings reviewed, only one mentioned the impact of new restrictions on surprise billing but reported that no adjustment was made for it. None of the insurers reviewed mentioned the impact of the administrative fix to the “family glitch” in their filings.
Discussion
Similar to last year, it appears that 2024 rates may rise moderately. The median proposed rate increase is 6% nationally, with most proposed increases falling between 2% and 10%. Most enrollees in this market are subsidized and do not pay the full premium. However, premium increases can affect federal spending and the driving factors behind these increases illustrate broader trends driving health costs in 2024.
A key driver of the increase in premiums in 2024 appears to be rising health prices. While prices for health services tend to grow every year, it also appears that inflation in the rest of the economy may now be starting to flow into the health sector. Rising prices and utilization are not necessarily specific to the ACA individual market. Similar levels of medical trend were observed in small group market filings as well.
Many insurers that publicly quantified the impacts of the pandemic are projecting a decrease in COVID-19 related costs in 2024. There are multiple factors considered when evaluating the total impact of COVID-19 on costs. Some insurers mentioned higher costs associated with vaccine costs shifting to insurers. Resumed member cost-sharing for COVID-19 testing, however, may have a downward effect on premiums as members seek out these services less due to their cost.
Relative to inflation and the pandemic, fewer insurers mentioned the impact of the unwinding of the Medicaid continuous enrollment provision, and there was variation in how insurers project its impact on costs. A very small number of insurers mentioned the upward effects of diabetic therapy and weight loss drugs on pharmaceutical trends, mostly pointing to increasing costs and utilization of said drugs. Federal policy changes, like the administrative fix to the Family Glitch and the No Surprises Act, were rarely mentioned by insurers, if at all, despite their potential impacts on enrollment and costs.